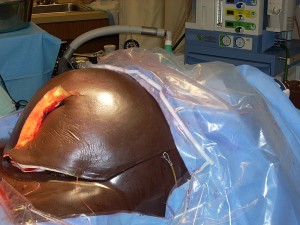
A doctor at Drexel’s College of Medicine has helped to create the first cesarean section “manikin” that will save lives through realistic C-section simulation training in developing countries. The simulation, dubbed “C-Celia,” will teach health professionals how to perform emergency surgical interventions in areas of the world where neonatal and maternal mortality rates are extremely high.
“This is truly a first-in-the-world simulation and a design to save lives,” Dr. Owen Montgomery, chair of the Department of Obstetrics and Gynecology at Drexel’s College of Medicine, said. “There are birthing simulators, which are not very lifelike, but there are no other simulators that allow you to do what we do.”
C-Celia was brought to Montgomery by colleague Dr. Robert Buckman in February 2011, who created the prototype and asked Montgomery if he could train people to use it. In July of that year, the simulation won first place in the Saving Lives at Birth category for the Grand Challenges in Global Health Grant.
As a lifelike model of a pregnant woman in need of a C-section, C-Celia prepares health professionals for what they will see in the operating room. An operator will need to cut through C-Celia’s abdomen, uterus and placenta to retrieve the model infant inside. C-Celia is also designed so that a single person can perform the operation alone, which may be the case in areas of the world where trained professionals are scarce. This is done with the use of a plastic ring retractor that keeps the abdominal incision open.
People are trained on C-Celia in small tasks. An operator will first be taught to make a skin incision and do so multiple times until he or she is proficient. Only after mastering skin incisions will the operator be able to move onto the next step of the surgery. Once proficient in all steps involved in performing a C-section separately, the operator will actually get to deliver the baby on C-Celia. Training in this way cuts down on costs, as the parts of C-Celia that get destroyed by incisions need to be replaced.
This simulated operation will need to be done while wearing gloves because the model features fake blood and amniotic fluid. Additionally, C-Celia can be adjusted to create difficult birthing situations.
“We can actually teach complicated deliveries by putting a baby in the uterus in different positions, so you have to know the different mechanisms to try to get a difficult baby out. We can make the model bleed, requiring the surgeon to know how to repair ruptures and bleeding lacerations,” Montgomery said.
C-Celia can also train an operator on how to perform a hysterectomy, a feature that will be used primarily in the U.S. The simulation’s main purpose is to instruct nonobstetricians, such as midwives and other health technicians, on how to carry out a lifesaving emergency C-section.
According to the World Health Organization, over half a million women die every year in pregnancy and childbirth in the developing world, and many of these deaths occur in Africa. This is where Montgomery saw a need for intervention in maternal and neonatal care, citing what he referred to as the three delays in delivery that lead to these subsequent deaths — the delay in deciding to seek care, reaching care and receiving care.
Reaching care proves extremely difficult in some countries where the two- to four-hour ambulance ride increases the mortality rate up to 50 percent. Though these countries often have small, local hospitals and clinics, distant university hospitals are the only places that offer emergency measures such as C-sections.
“We had resources and needs that weren’t mixed well. I believed I could train whoever was there rather than putting a woman into an ambulance and having her bleed to death on the way to the hospital. There are a couple of small hospitals around [The Gambia], but there are no providers of emergency obstetrics. They have midwives, and they can do routine obstetrics, but not complicated obstetrics,” Montgomery said. “So if we could teach one of the providers right there how to do a lifesaving cesarean delivery, even if they’re not an obstetrician, we could save two lives —the mom’s and the baby’s.”
Teaching local village technicians how to perform C-sections with the simulator has additional benefits. Nonphysicians trained locally have a much higher chance of remaining with the village clinic or hospital than do physicians, who will often leave after being trained.
“You’re not maintaining the ability to perform lifesaving deliveries by training the very few physicians there are because they go back to the capital or the United States to do something else,” Montgomery said.
In a country like the U.S., where the infant mortality rate is only 14 per every 100,000 births, teaching physicians to deliver with C-Celia is less purposeful. However, these skills, when taught to midwives and other nonphysicians, can be used when they go to developing countries.
“You have to go to where it is that you’re doing the most good. You can help women in Philadelphia, and we do every day, but we can’t have the same level of impact in Philadelphia by adding this technique because every hospital in Philadelphia is already fully capable and ready to go. Of course I can train the doctors here better, and I can train them in emergencies they don’t see all the time. But if 99 percent of the deaths occur in Africa, you have to go to Africa,” Montgomery said.
C-Celia has been used in simulations of natural disasters and extreme emergencies to prepare operators for worst-case scenarios. During an on-campus simulation day April 30, teams of students had to deliver a baby with C-Celia after the event of a simulated car accident. The objective of the operation was to intervene and save both mother and child at a time when the mother’s vital signs were fine and encouraged teamwork among the students.
“We teach as a team because when you go into the world, you’re going to practice as a team. So it’s entirely possible for medical students to learn all of their medical stuff and nurses to learn all their nursing stuff, and the first time they ever work together, they’re actually treating real patients. Well, that’s not the best method,” Montgomery said. “So what we want to do is to train people to work in the teams they’ll be working in later on because that will actually improve quality and satisfaction and safety. We use simulation as a vehicle to put teams together to train.”
Montgomery has met with several universities abroad that wish to work with C-Celia. He has also spoken to world leaders such as the first lady of Zambia, Dr. Christine Kaseba-Sata, who is an obstetrics and gynecology specialist herself and wants the model to be used for training in her country.
“Every once in a while, what I’ve learned and how I practice will save a life, and that is the absolute most rewarding thing. I can’t save lives if I’m not there, but I can teach people who can save lives every day,” Montgomery said.
Montgomery predicted that C-Celia will be ready to use for training in Africa within the next 12 months.