Dr. Wei-Heng Shih of the Materials Science and Engineering Department and Dr. Wan Shih from the School of Biomedical Engineering are working to revolutionize the way surgeons remove tumors from patients on the operating table. By using quantum dots, the small particles that power televisions, they are able to light up cancer cells and help surgeons determine whether or not they have managed to remove the tumor completely.
“We’ve been synthesizing quantum dots,” Wei-Heng Shih said. Looking for an application in the medical field, he found one when he and his wife worked with surgeon Harry Brooks of the College of Medicine. Brooks complained that he didn’t know whether or not he’d removed the entire tumor.
“It occurred to us that it could be a good application to solve this problem in surgery,” Wei-Heng Shih recalled.
Currently, when surgeries are done, especially for patients of breast cancer, one of the goals of the surgery is to minimize the amount of tissue removed.
Wei-Heng Shih described the primary issue, “You want to make sure you remove all of the tumor, so you try to remove as much as possible, however…you don’t want to take out too much.This kind of surgery is a little different,” he said, referring to breast-conserving surgery. To avoid a full mastectomy, or removal of the breast that has cancerous tissue, the goal is to remove the tumor with a thin layer of healthy cells — enough to ensure that the tumor is removed, but keep as much healthy tissue in tact as possible. “It’s kind of a conflicting requirement, so different surgeons will handle it differently…that leads to a big problem in surgery,” he expanded.
The big problem surgeons face is the risk of remission. Cancer cells, unlike normal cells, don’t have the checks on growth that they should. Instead, they continue to grow and divide when growth should have ceased. Meaning it takes a single cancerous cell remaining for someone in recovery to become a patient again.
“A lot of patients did not have the cancer removed completely, so they have to come back for another surgery,” Dr. Wei-Heng Shih explained, a phenomenon known as the resection rate. When discussing breast cancer specifically, he said, “On average, we’re talking 25-60% resection rate,” meaning that anywhere from a quarter to just over half of breast cancer patients require a second surgery to remove more cancerous cells.
Dr. Wei-Heng Shih continued, explaining the problems associated with that second surgery, “A second surgery costs money, causes pain, and a second surgery is correlated with a higher rate of metastasis.” The last of those problems is perhaps the most dangerous one for many patients. Metastasis — the spread of a cancer from one part of the body to another — could cause an otherwise harmless or easier to treat cancer to become particularly dangerous and life threatening, meaning it’s imperative that surgeons removing tumors attempt to do it with the least number of surgeries possible. “Our goal is to minimize [the need for] this second surgery,” he continued.
Minimizing the need for the second surgery is where those quantum dots come in. “Our solution is to use a molecular probe to see whether the tumor is completely removed, if there are any cancer cells remaining, if the surgery is clean,” Wei-Heng Shih said. The process can be done in the surgery room before the patient is stitched back up.
“They’ll take out the tumor, and then immerse it in this solution with the molecular probe. We take it out, then put it on the imaging table, and shine light on it. A detector will take an image of the light,” Wei-Heng Shih explained.
Wan Shih detailed further, “After binding in the solution, you will image it in near-infra red light, so it’s very clean.” The word — clean — is extremely important when it comes to cancer surgery. When the difference between a patient’s near-guaranteed survival or death sentence is a mere layer of cells, ensuring that a tumor is removed cleanly is critical.
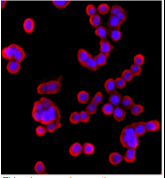
Wan Shih explained the results that he and Wei-Heng Shih want to see, “If the computer screen is all dark, then it’s clean, but if the computer screen lights up, it’s not clean.” The goal is to have a minimal layer of healthy cells surrounding the tumor to make sure it’s all removed – if all the cells are healthy, nothing should light up. If the image of the tumor lights up, that means that there is a risk that cancer cells are still in the body — a risk that a surgeon is not willing to take.
Both went on to explain the process of causing cancer cells to light up, or fluoresce, on the molecular lever. Wei-Heng Shih began with the nanoparticles, the quantum dots. “They are excited with another light — this is called photoluminescence. The particle is excited by a light, causing it to emit a different light.” While this concept is the basis for their technology, to allow it to check on cancer cells, an addition had to be made.
“We put an antibody linked to the particle, what we call a molecular probe,” Wan Shih said. “The marker we use is the sugar of a glycoprotein. It is very effective in differentiating cancer from normal tissue,” he continued.
Cancer cells are unique from normal cells in many ways — one such way is the production of glycoproteins unique to cancer cells. A glycoprotein is a molecule that has one part that is a sugar (the “glyco” part) and one part that is a protein. The two professors use these unique molecules to tag cells that have cancer with particles that glow.
Wei-Heng Shih and Wan Shih are hopeful for what the future brings. Their immediate focus is doing more research to understand more about how these work — they want to collect more data, begin clinical tests and have submitted a proposal for funding from the National Institutes of Health. They hope that these techniques can be applied to other cancers beyond breast cancer, including diseases of the brain, face and any disease that would require invasive surgery, where you want to avoid removing too much tissue. They also hope that their technology could be used in gene therapy, making it easier to deliver genes and treat various genetic disorders and be sure that the gene gets to its destination by being able to watch it light up.


